Screenings · ABCDES Longevity Framework
Screen Early. Prevent Disease. Protect Your Future.
Screening is the foundation of preventive health. Most chronic diseases begin silently for years before symptoms appear. Screening allows us to identify risk early and take action before damage occurs—often decades before disease is diagnosed.
Up to 80% of chronic disease deaths are preventable when the right screenings are done early and followed by targeted action.
Course by Dr. Daniel L. Beckles · Educational only · Not a substitute for personalized medical care.
ABCDES Longevity Circle
Screening is the “S” at the center of the ABCDES system—connecting A1C, Blood Pressure, Cholesterol, Diet, Exercise, Stress, Sleep, and Stop Smoking into one measurable loop.
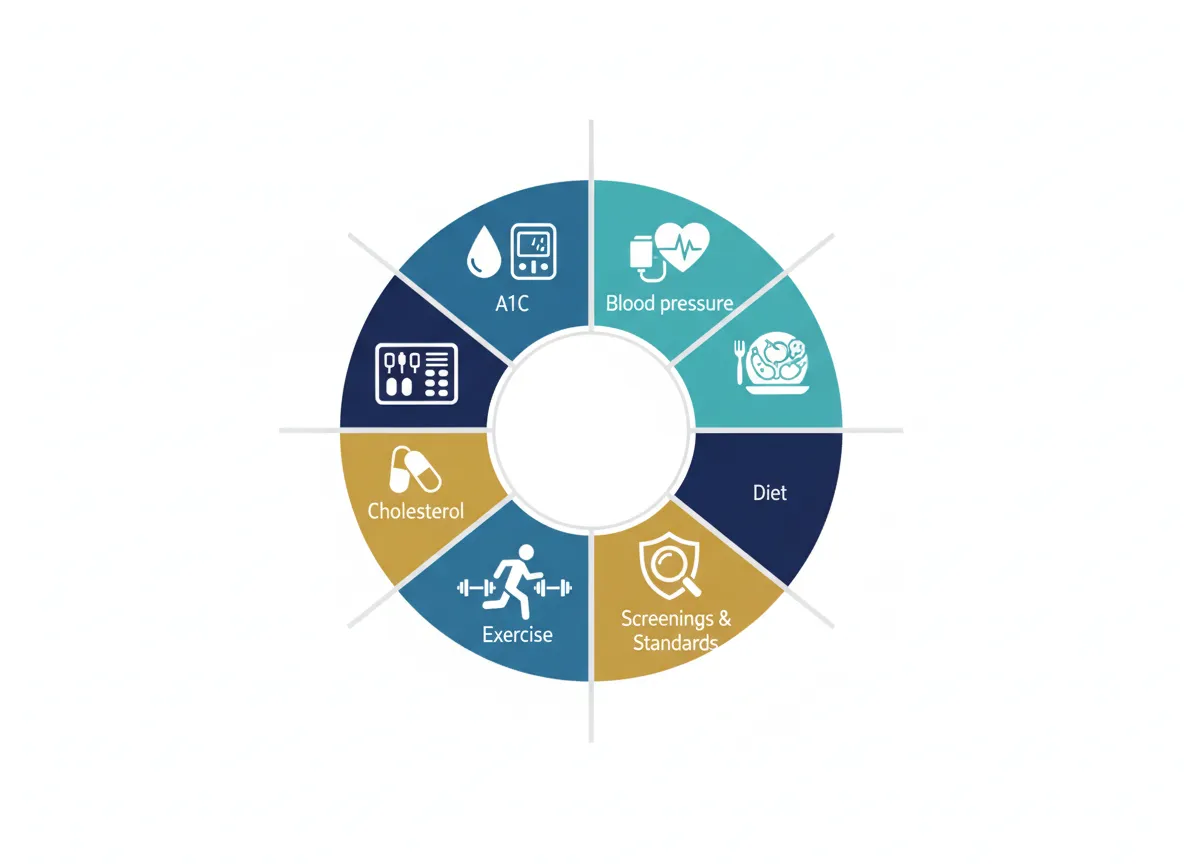
In the Screenings module of the course, you’ll learn exactly which tests to ask for, when, and why—so you can have more informed conversations with your healthcare team.
What Is Screening?
Screening means finding disease before symptoms appear.
Screening is the process of testing for disease before symptoms develop. Once symptoms appear, you are already in the diagnostic and treatment phase—often years or decades after silent damage began.
Screening is performed when a person:
- has no symptoms
- has no abnormal exam or clinical findings
- appears generally healthy
The purpose of screening is early detection. Early detection allows intervention before downstream disease develops—when lifestyle, medications, or procedures can have the biggest impact.
Screening vs. Diagnosis
Screening: You feel well. No symptoms. You check anyway.
Diagnosis: You feel unwell. Symptoms are present. You are already late in the process.
Course insight: In the Screenings module, you’ll learn how to turn a 15-minute annual visit into a powerful prevention strategy by asking for the right labs and imaging early.
Why Screening Matters
Most chronic disease begins silently.
Heart disease, stroke, diabetes, and many cancers develop over years or decades before symptoms appear. By the time you feel something, your biology has been changing quietly in the background.
Research from organizations like the U.S. Preventive Services Task Force, CDC, and World Health Organization shows that early detection through preventive screening can significantly reduce disease burden and premature death.
Screening allows people to:
- detect risk early
- intervene earlier, when changes are most effective
- reduce complications and hospitalizations
- improve long-term healthspan and lifespan
Visual Insight
- 1. Silent changes in blood sugar, blood pressure, cholesterol.
- 2. Organ stress in the heart, brain, kidneys, eyes.
- 3. Visible disease — heart attack, stroke, dialysis, disability.
Screening moves you back up the ladder—catching risk while it is still reversible.
The ABCDES Screening Framework
What should you be screening for?
The ABCDES Longevity Framework organizes preventive screening into measurable categories you can track and improve over time.
A — A1C (Blood Sugar)
What it measures: Average blood sugar over three months.
Why it matters: High blood sugar damages blood vessels, nerves, kidneys, and eyes.
Normal range: Below 5.7%.
Why screening matters: Prediabetes often develops silently for years—early detection can prevent progression.
B — Blood Pressure
What it measures: The pressure of blood flowing through arteries.
Normal range: Around 120 / 80.
Why screening matters: High blood pressure is the “silent killer”. It can cause stroke, heart attack, and kidney disease without symptoms.
C — Cholesterol
What it measures: Blood lipids that influence plaque formation in arteries, including LDL, HDL, and triglycerides.
Why screening matters: Uncontrolled cholesterol contributes to ischemic heart disease, stroke, and peripheral artery disease—often before any warning signs.
D — Diet (Behavior Screening)
Diet is a screening behavior indicator. Your day-to-day eating patterns provide insight into metabolic risk long before lab tests change.
Screening questions include:
- How often do you eat processed foods?
- How many servings of fiber-rich plants do you eat daily?
- How frequently do you drink sugary beverages?
E — Exercise (Movement Screening)
Physical activity level is a critical longevity indicator. Movement patterns can be screened long before disease appears.
Screening questions include:
- What is your average daily step count?
- How many minutes per week do you exercise?
- How many hours per day are you mostly sedentary?
Beyond Blood Tests
The Four S's of Screening
Screening isn’t only labs—it includes cancers, mental load, sleep quality, and nicotine exposure.
Screening for Cancer
Cancer screening looks for cancer or precancerous changes before you notice symptoms. Examples include:
- Colon cancer screening (e.g., colonoscopy, stool tests)
- Breast cancer screening (e.g., mammography)
- Cervical cancer screening (e.g., Pap test, HPV test)
- Prostate cancer discussions and PSA testing based on risk
Guidelines vary by age, sex, family history, and personal risk. The course walks through how to use resources like the U.S. Preventive Services Task Force to personalize a screening plan with your clinician.
Screening for Stress
Chronic stress raises cortisol, blood pressure, and metabolic disease risk. Screening for stress includes brief questionnaires, burnout scores, and heart rate variability trends.
Screening for Sleep
Poor sleep affects metabolism, cognition, mood, and cardiovascular health. Sleep screening can include sleep duration, snoring, apnea risk, and wearable data.
Screening for Smoking & Nicotine
Smoking and vaping damage blood vessels, lungs, and increase cancer risk. Simple questions about cigarettes, cigars, vaping, and secondhand exposure help identify who needs support to quit.
The Cost Equation
Prevention is almost always cheaper than treatment.
Cost of Screening
- Many screenings are covered by insurance.
- Often $0 out of pocket during preventive visits.
- Basic tests frequently available for under $100.
Examples:
- A1C test — ~$20
- Cholesterol panel — ~$20
- Blood pressure check — often free at pharmacies or clinics
Cost of Untreated Disease
Late-stage disease may involve:
- Hospitalizations and intensive care stays
- Major surgeries or procedures
- Chemotherapy, radiation, or immunotherapy
- Dialysis for kidney failure
- Lifelong medications and frequent specialist visits
Total costs can reach hundreds of thousands to millions of dollars over a lifetime—but the greatest cost is often lost health and lost time with the people you love.
The Lottery Ticket Analogy
If you pay for insurance but skip screening, you’re not cashing in your ticket.
Most people already pay for health insurance through their paycheck or monthly premiums. Built into those premiums are preventive screening benefits—often at no additional cost.
Not using those benefits is like buying a lottery ticket and never checking the numbers. The money has already left your account—but you never discover the potential payout.
Screening allows you to cash in the ticket. The prize is not cash—it’s extra healthy years of life and more time with the people you care about.
Bring the ABCDES worksheet from the course to your next visit so you don’t miss key screenings.
The Longevity Loop
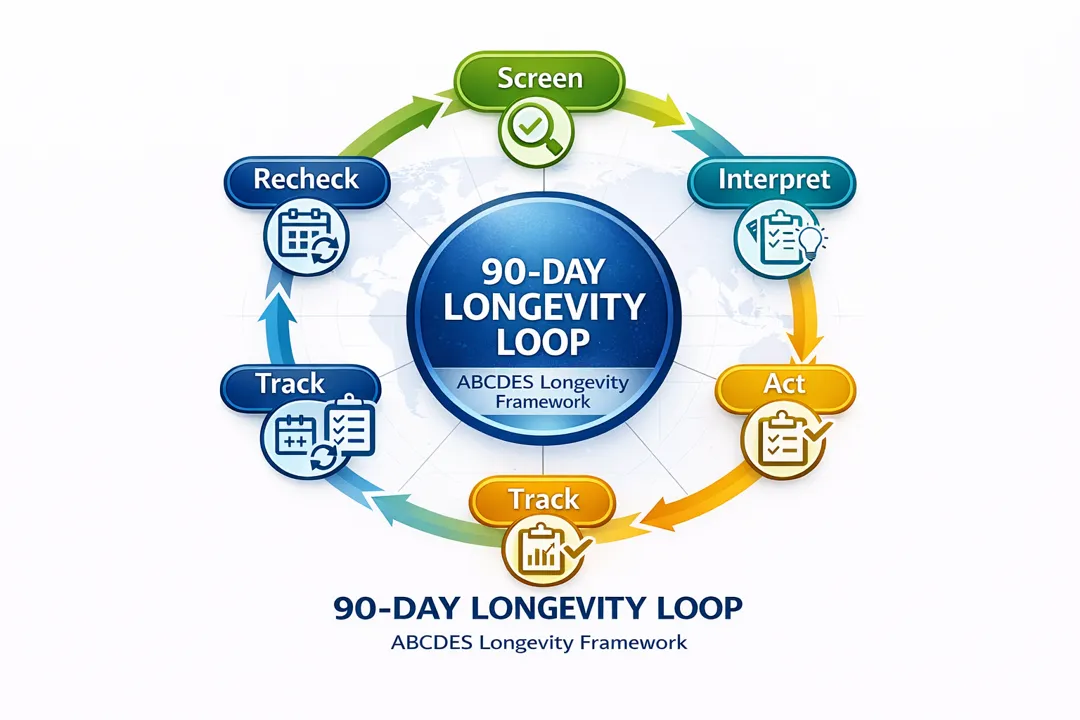
Screen → Interpret → Act → Track → Recheck.
Screening is not a one-time event. It is the first step in a loop that repeats every few months or years, depending on your risk and results.
- Screen: Get the right tests at the right time.
- Interpret: Understand what your numbers mean.
- Act: Adjust lifestyle, medications, or environment.
- Track: Watch trends, not one-time results.
- Recheck: Repeat the right screenings on schedule.
The ABCDES course gives you plug-and-play scorecards and trackers so that you can run this loop for A1C, blood pressure, cholesterol, weight, sleep, and more.
What to Screen, When
Decade-by-decade screening roadmap
Use this as a conversation starter with your healthcare professional. Exact timing depends on your sex, family history, and national guidelines (CDC, USPSTF, WHO, NIH).
20s–30s
Core screenings:
A1C or fasting glucose if at risk for diabetes.
Blood pressure (at least every 3–5 years, more often if elevated).
Cholesterol/lipid panel (timing based on risk and guidelines).
Weight, BMI, and waist circumference (rule out metabolic syndrome).
Cancer-related screening discussions:
- Cervical cancer screening (Pap test / HPV testing per guidelines).
- Skin checks for changing moles (self-exam + clinical as advised).
- Family history review for early-onset cancers (breast, colon, etc.).
40s
Cardiometabolic focus:
Regular A1C/glucose, blood pressure, and cholesterol, screening.
Formal cardiovascular risk assessment (using validated calculators).
Weight, BMI, waist circumference, and lifestyle review.
Cancer-related screening discussions:
- Breast cancer screening (e.g., mammography) timing based on age and risk.
- Cervical cancer screening per updated guidelines.
- Skin, thyroid, and testicular or breast self-awareness exams.
- Family history–driven conversations about earlier colon or breast screening when appropriate.
50s
Core screenings:
- Ongoing monitoring of A1C, blood pressure, cholesterol, weight, and waist size.
- Colorectal cancer screening (e.g., colonoscopy or stool-based tests) starting at guideline-recommended ages.
- Bone health discussions (osteoporosis risk) depending on sex and risk.
Cancer-related screening discussions:
- Breast cancer screening (mammography at intervals based on guidelines).
- Prostate cancer screening discussions (PSA testing) based on individual risk and shared decision-making.
- Lung cancer screening (low-dose CT) discussions for eligible current or former smokers.
- Continued cervical cancer screening as indicated.
60s
Cardiometabolic and functional focus:
- Regular monitoring of blood pressure, A1C, cholesterol, kidney function, and medications.
- Gait, balance, and fall-risk assessments.
- Hearing and vision checks.
Cancer-related screening discussions:
- Continued colorectal cancer screening until guideline age cutoffs.
- Breast cancer screening intervals individualized based on health status.
- Prostate cancer screening discussions where appropriate.
- Lung cancer screening eligibility review in current/former smokers.
- Skin and other site-specific cancer checks as indicated by risk.
70s
Healthy aging focus:
- Ongoing monitoring of cardiometabolic health (A1C, blood pressure, cholesterol, kidney function).
- Cognitive, mobility, and fall-risk screening.
- Medication review for polypharmacy risks.
Cancer-related screening discussions:
- When to continue or stop colorectal, breast, cervical, or prostate screening based on overall health and life expectancy.
- Ongoing lung cancer screening for those who remain eligible.
- Skin cancer and oral cancer checks where risk factors exist.
80s and beyond
Goal-oriented screening:
- Focus on quality of life, function, and independence.
- Screening decisions individualized based on health, preferences, and projected benefit.
- Emphasis on symptom awareness, comfort, and shared decision-making around new tests.
Cancer-related screening discussions:
Many guidelines recommend stopping routine cancer screening at a certain age or when life expectancy is limited. At this stage, conversations focus on what feels most important to you—time, comfort, and personal goals.
Take the Next Step
Know your numbers today.
Use the ABCDES tools to turn this page into action with your healthcare team. Start with one small step—then build your longevity plan over time.
Ready for a deeper dive? The ABCDES Longevity Program is a six-week course that teaches you how to interpret your numbers and build a 90-day correction plan with your clinician.
References & Guidelines
Built on evidence, not opinion.
Screening recommendations change as new data emerges. Always check up-to-date national guidelines and review them with your healthcare professional.
Key resources for evidence-based screening:
Important: This site and course are educational only and do not replace personalized medical advice, diagnosis, or treatment. Always discuss screening decisions with a qualified clinician who knows your full history.
ABCDES Longevity Framework
A measurable, actionable system to understand your numbers, partner with your clinicians, and prevent downstream disease wherever possible.
Medical Disclaimer
Content is for educational purposes only and should not replace medical advice from a qualified healthcare professional. Do not start, stop, or change any treatment based solely on this information.
© 2026 Screenings · ABCDES Longevity Framework.